ARPA Increases COBRA Access: Impacts for Employers
The American Rescue Plan Act of 2021 expands Cobra access to millions
How does this affect your business?
When the American Rescue Plan Act (ARPA) was signed into law on March 11, 2021 all eyes were on the economic stimulus payments. Who would be eligible? How much would the third round of checks be worth? When would payments be sent out? However, there is much more to this bill than direct payments, some of which employers should be paying direct attention to in order to avoid economic surprises.
What’s Going on With COBRA?
Effective April 1, 2021 through September 30, 2021 the government will subsidize 100% of COBRA premiums for certain terminated workers, certain workers who have had their work schedules reduced, and their eligible dependents.This unprecedented act helps guarantee that certain employees who were involuntarily terminated or had their hours reduced and lost health plan coverage during the pandemic are eligible to maintain (and in some cases change, if the employer permits) the level of health coverage they had while employed, without stressing their finances.
To pay for this coverage, the government will be providing a quarterly payroll tax credit to reimburse employers who will incur the initial cost of providing this subsidized COBRA coverage. Employees are eligible for this subsidized COBRA coverage if they were involuntarily terminated or if a reduction of hours caused them to lose health coverage dating back to November 2019 (more on this later). If an employee left a position voluntarily, they are not eligible for this benefit.
Who is Eligible for ARPA COBRA Subsidies?
First of all, let’s start with the basics: what even is COBRA?
COBRA creates a safety net for terminated employees to remain insured for health coverage while they seek another job or different insurance options. Before ARPA, the premiums for COBRA coverage would have to be paid in full by the former employee, instead of splitting the cost with an employer as is typical practice. This can be incredibly expensive, especially considering people using COBRA don’t typically have a stable source of income to fund these insurance premiums.
Now under ARPA, eligible employees will qualify for free COBRA coverage for all, or a portion of, the period commencing April 1, 2021 and ending September 30, 2021.
Those eligible for this coverage are:
- Individuals who were involuntarily terminated from their jobs or had their hours of service reduced, causing a loss of health coverage, dating back to November 2019 and who have not yet enrolled in coverage or enrolled in coverage and subsequently cancelled their coverage
- Individuals who currently no longer qualify for employer-sponsored healthcare coverage due to an involuntary termination of employment or reduction in working hours and currently are eligible to elect COBRA
- Individuals who are already enrolled in COBRA coverage as of April 1, 2021 and wish to continue with their coverage.
- Individuals who currently have employer-provided health coverage, but are involuntarily terminated or have their hours reduced, causing them to lose health coverage between April 1 and September 30, 2021.
*Note: these eligibilities do NOT cover individuals who lost their coverage due to a voluntary termination.
COBRA coverage generally has a maximum period of 18 months, and ARPA does not extend this period, even if it ends before September 30, 2021. Additionally, individuals are required to notify their employer or insurance provider as soon as they become eligible for other coverage during this subsidy period. Failure to do so can cost individuals a penalty of $250 and up to 110% of the subsidy cost that was wrongfully provided to them.
ARPA 2021 Timeline
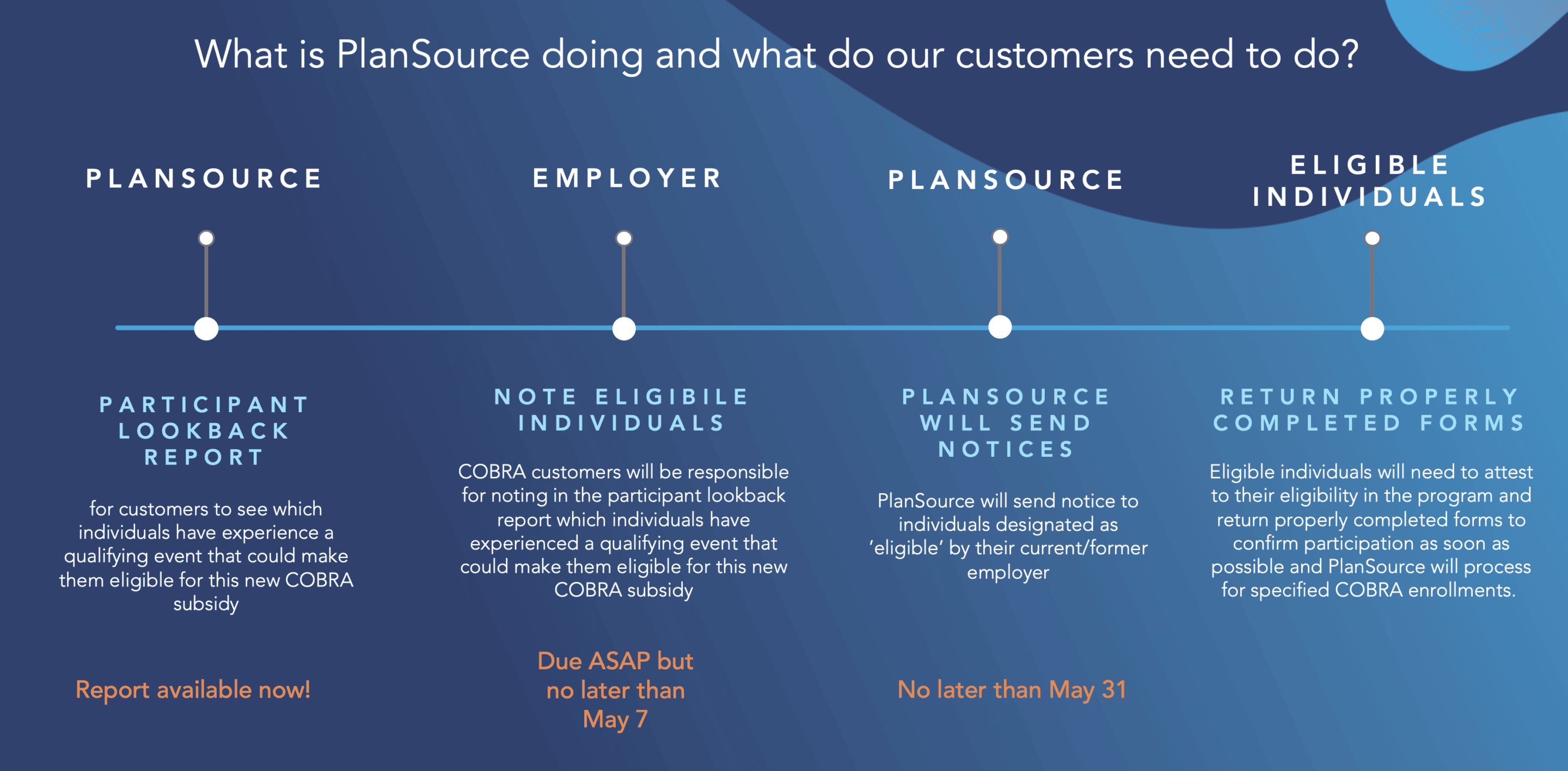
What Employers Need to Know About ARPA & COBRA
Employers should brace themselves for a heap of administrative work in the coming weeks. Though specific details of this subsidy may not be released by the Department of Labor until April 10, 2021, we do have plenty to digest from the actual law itself. Both employers and their COBRA administration vendors should be aware of the following to ensure they remain compliant and avoid the risk of financial penalties:
- Track your COBRA subsidy amounts – Whether you administer COBRA in-house or outsource it, track your payments. Do this meticulously so you can ensure you receive proper credits to recoup the cost. Then work with your payroll provider to claim your refundable tax credit as necessary.
- Be cognizant of election change requests – Employers need to work with their insurance carriers to decide whether or not they will allow election changes. The changes can only be an alteration to a lower-cost insurance coverage and the decision to allow such changes is completely at the employer’s discretion.
- Provide subsidy notice to eligible employees – Employers or their COBRA administrator need to provide new notices to those eligible for this subsidy. (Additional info below, but more detailed information will be available from the Department of Labor in April.)
- Audit for the ‘special enrollment window’ – This one is tricky but must be completed by May 31, 2021. Employers need to look back to November 2019 to identify qualified employees, spouses, and dependents who may still be entitled to elect COBRA and notify them of the special enrollment opportunity.
For customers that have COBRA services with PlanSource rest assured, that we will send out the required notices and administer any enrollments, terminations and changes. Interested in outsourcing your COBRA headaches to our experts? Chat with our team!
If you have questions for our COBRA team regarding this new legislation please reach out to your PlanSource Customer Success Manager or email cobra.arpa@plansource.com. As always with new legislation PlanSource will be communicating with customers on next steps and the process.
What Are These New COBRA Notice Requirements for ARPA?
The prerequisite to this aspect of ARPA is that all employers must provide notice of the COBRA subsidy to qualified individuals in a timely manner. More specific details of these notification requirements will be coming next month from the Department of Labor, but we currently know the following:
- New Requirement Notices – Employers must notify individuals who become eligible for the COBRA subsidy about its availability from April 1 through September 30, 2021 as well as their option to change to a lower cost-plan if the employer allows it.
- 60-Day Special Election Period Communication – By May 31, 2021 employers need to have audited their employee records back to November 2019 and notify all individuals who are eligible for the COBRA subsidy and who became eligible for COBRA coverage before April 1, 2021, including those who chose not to elect it, or terminated it early, that they are eligible again through ARPA.
- Provide Notice of COBRA Subsidy Expiration – At least 15 days prior to the expiration of an individual’s COBRA subsidy, but not more than 45 days prior to such expiration, an employer must notify an employee that theCOBRA subsidy is coming to an end. This notice does not have to occur if an individual’s coverage ended because they became eligible under another plan or because their COBRA coverage otherwise ended due to the completion of the COBRA period.
The Takeaways
A recent Forbes study on COVID job impacts warns that it could take up to 4 years to recover the 22 million jobs that were lost due to the pandemic, and while the American Rescue Plan Act can’t speed up job recovery, it can work to soften the blow to the affected workforce. With ARPA, many Americans will once again have the ability to protect themselves and their loved ones by having access to the benefits they qualified for before being terminated or losing their hourly status since November 2019. This is a huge lifesaver for employees, but an equally huge administrative headache for employers.
It is highly recommended that employers work closely with their COBRA experts, whether in-house or outsourced, to ensure they are being compliant with the new law per the requirements above or risk financial penalty. The details of the plan can get complicated quickly, and it will be crucial to stay on top of the continued guidance which will come from the Department of Labor in the coming weeks.
As we all move forward toward life after the pandemic, it’s important that we do so together and embrace acts like ARPA to ensure those adversely affected by the pandemic have the coverage and security they deserve.
The information contained in this site is provided for informational purposes only and should not be construed as legal or professional advice on any subject matter.
You should not act or refrain from acting based on any content included in this site without seeking legal or other professional advice. The contents of this site contain general information and may not reflect current legal developments or address your situation. PlanSource disclaims all liability for actions you take or fail to take based on any content on this site.
Empathy, Innovation & Action: Top Takeaways from HR Leaders Who Spoke at Eclipse
Empathy, Innovation & Action:Top Takeaways from the HR Leaders Who Spoke at...
Charting the Future of PlanSource: Our Vision for What’s Ahead
Discover how PlanSource unveiled game-changing AI innovations at Eclipse 2025, transforming how HR leaders manage benefits and how employees choose them. The future of benefits starts here.
Navigating New Requirements with the Paperwork Burden Reduction Act
Navigating New Requirements with the Paperwork Burden Reduction...




