Automate Your Most Time-Consuming Tasks
25%
48X
5 HOURS
40%
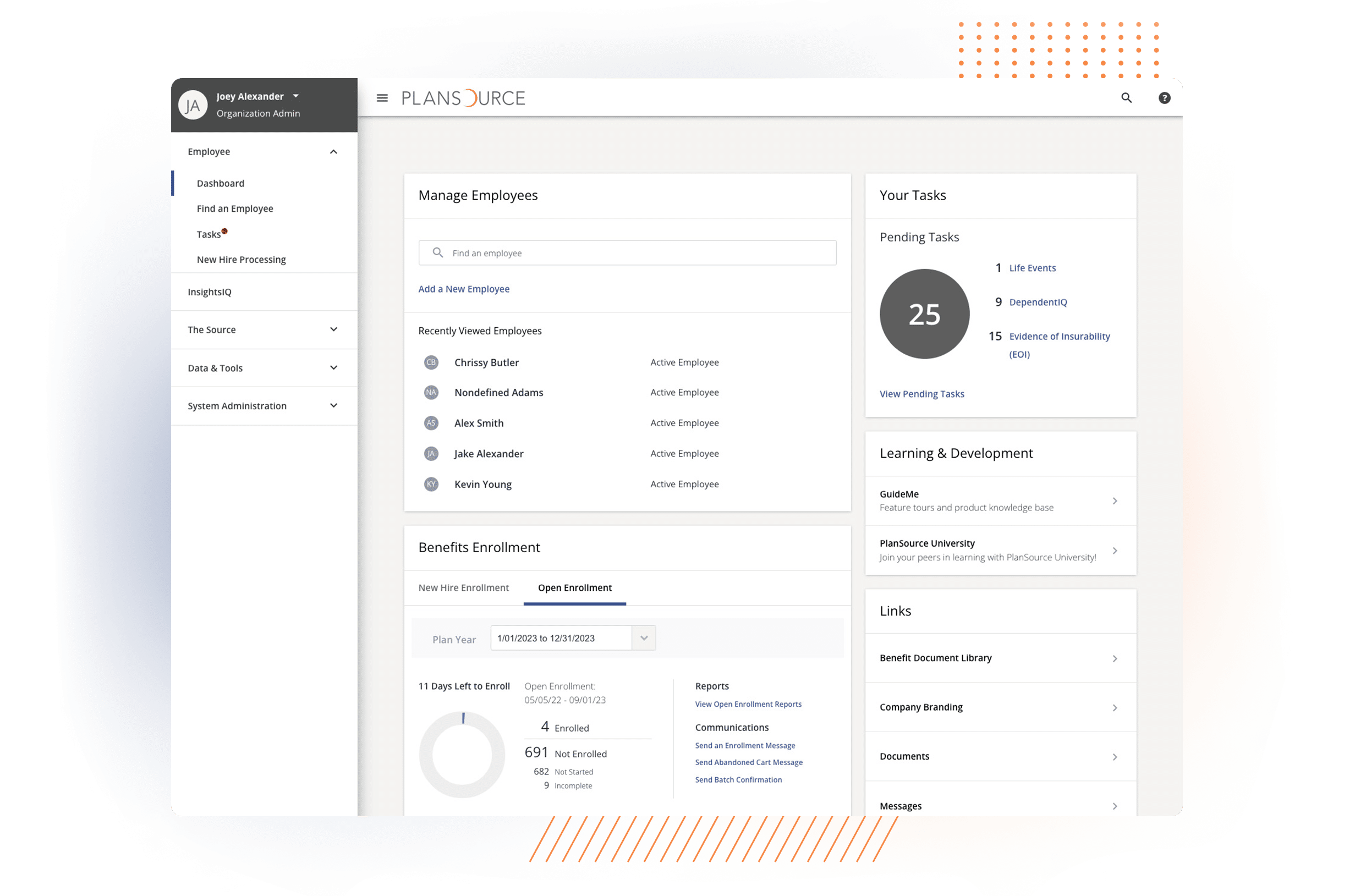
ACA MEASUREMENT & REPORTING
BENEFITS REPORTING
BILLING RECONCILIATION
ELIGIBILITY MANAGEMENT
EOI
LIFE EVENT CHANGES
NEW HIRE ENROLLMENT

Simplify Your Most Complex Benefits Setups
Workforce Populations
Define your company’s unique employee groups where rules vary
Cost Contributions
Designate employee and employer contributions to benefits premiums
Automated Enrollment
Enroll employees in company-sponsored benefits by default
Get Started

Benefits Billing Reconciliation Demo

How to be Successful in Affordable Care Act Reporting and Compliance

